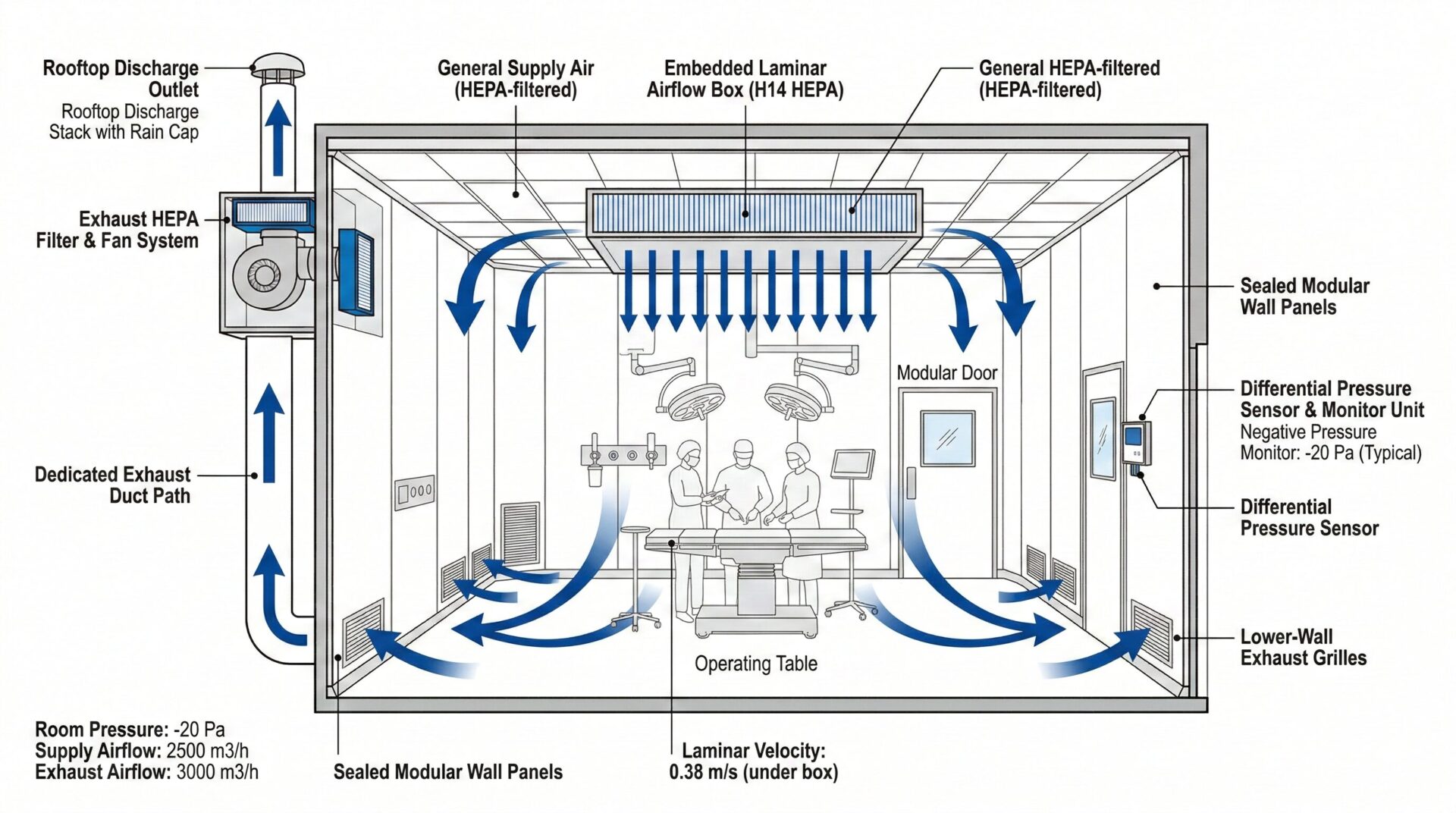
Negative Pressure Operating Room Design & Airflow Control Explained
Negative pressure operating rooms are often misunderstood. Many treat them as “the opposite of positive pressure theatres,” but the engineering objective is fundamentally different. A standard operating room is designed to protect the sterile surgical field; a negative pressure operating room is designed to protect the hospital environment by containing airborne contamination.
This guide breaks down the engineering logic behind negative pressure OTs: how negative pressure is created, how exhaust and filtration should be engineered, the “no return vs return” debate, pressure monitoring and recovery behavior, and how these requirements should be integrated into modular operating theatre systems.
1) Why Negative Pressure Operating Rooms Matter
Infection control in healthcare infrastructure is not limited to “keeping the operating room clean.” Certain procedures introduce airborne or aerosol risks that require a different ventilation strategy: instead of pushing air outward (positive pressure), the room must continuously draw air inward to prevent contaminated air from escaping to adjacent spaces.
Design intent difference: Positive pressure protects the patient and sterile field. Negative pressure protects the surrounding hospital environment by containing airborne contamination.
Negative pressure OTs are typically considered when hospitals require infectious-surgery capability, outbreak readiness, or high-risk aerosol-generating procedures. The result is a containment-driven room where exhaust, pressure monitoring, envelope sealing, and commissioning discipline become critical.
2) What Is a Negative Pressure Operating Room?
Definition and engineering meaning
From an engineering perspective, a negative pressure operating room is a surgical environment where the air pressure inside the room is maintained lower than adjacent spaces, ensuring airflow direction is always inward when openings or leakage occur.
Typical pressure range
- –5 Pa to –15 Pa relative to corridor or anteroom (exact setpoint depends on project standard and risk policy).
- Some projects implement a pressure cascade (corridor → anteroom → OT) to create layered containment.
How negative pressure is created
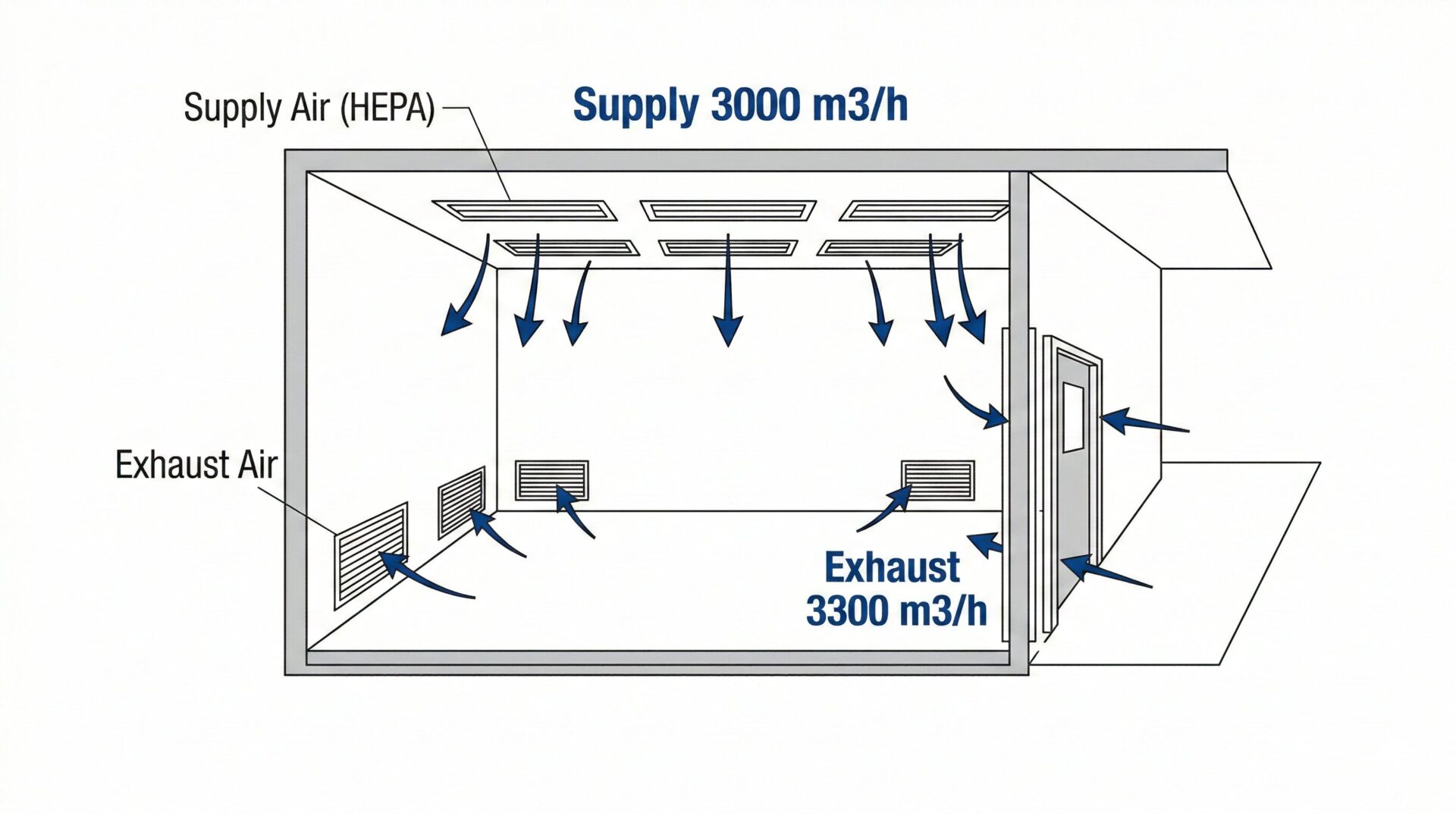
The governing rule is simple: exhaust airflow must exceed supply airflow. Example:
- Supply air: 3,000 m³/h
- Exhaust air: 3,300–3,450 m³/h
The difference is made up by controlled infiltration from adjacent spaces (door gaps, transfer grille, or defined leakage path), producing inward airflow and maintaining containment.
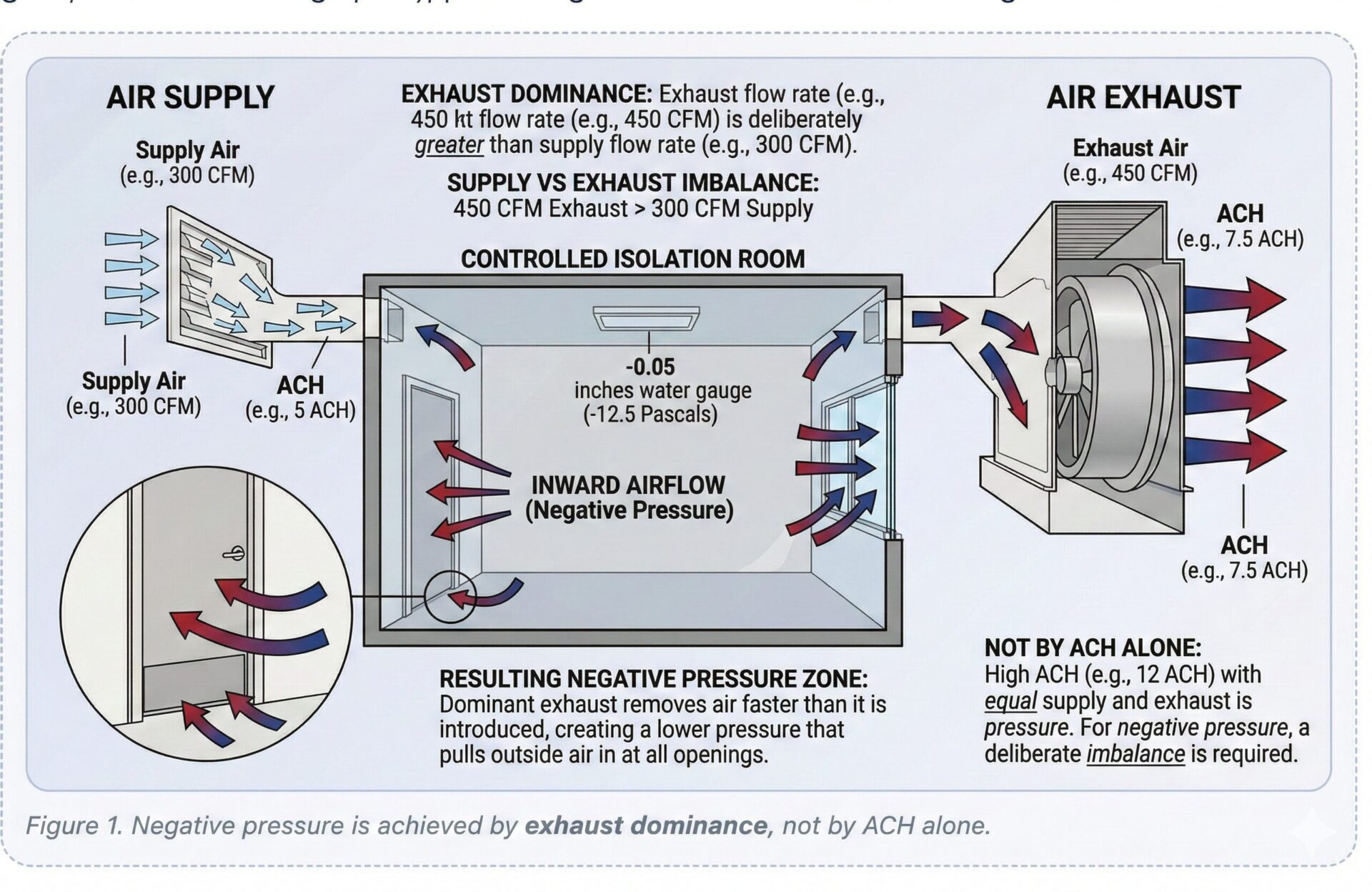
3) Core Design Principle: Airflow Must Always Move Inward
The core containment requirement can be summarized in one sentence: contaminated air must never escape the room. Negative pressure is therefore a system-level containment strategy, not a single HVAC parameter.
3.1 Airflow imbalance strategy
Negative pressure is typically maintained by designing exhaust airflow to be approximately 10–15% higher than supply airflow. This provides a stable inward airflow direction even during small disturbances.
3.2 Pressure cascade strategy
In higher-control designs, pressure is staged across adjacent spaces:
- Clean corridor: 0 Pa
- Anteroom: –5 Pa
- Operating room: –10 Pa (example)
This reduces cross-zone contamination risk and makes containment behavior more predictable during door operations.
3.3 Door leakage compensation
No room is perfectly airtight. Real performance depends on how the system compensates for expected leakage through doors, penetrations, and access panels. A robust design includes:
- Predictable leakage paths (not random cracks)
- Pressure sensors with feedback control
- Fast recovery after door opening events
Key takeaway: Negative pressure must remain stable under real operating conditions (door opening, filter loading, wind effects), not only in static balancing.
4) Airflow Organization Inside the Operating Room
Creating negative pressure is not enough. The internal airflow pattern must also protect the surgical field while capturing contaminated aerosols efficiently. In practice, negative pressure OT airflow must balance four goals: sterile-zone protection, contaminant capture, turbulence control, and thermal/humidity stability.
4.1 Ceiling supply air and downward flow
Most negative pressure OTs still use a controlled ceiling supply strategy (often laminar airflow) with high-efficiency filtration. Downward airflow supports the sterile field by pushing particles away from the critical zone.
4.2 Thermal plume behavior and aerosol movement
Surgical lights, equipment, and occupants generate heat plumes that can lift aerosols upward. Infectious aerosols may follow these upward currents, so exhaust placement must consider both downward supply patterns and upward plume capture zones.
4.3 ACH vs containment
Air changes per hour (ACH) improve dilution, but ACH alone does not create negative pressure. Think of the relationship as:
- ACH controls dilution (how quickly contaminants are reduced by fresh/clean air exchange)
- Exhaust dominance controls containment (inward airflow direction and pressure regime)
4.4 Avoiding short-circuit airflow
A common design mistake is placing exhaust in a way that pulls supply air directly into exhaust (“short-circuit”), reducing effective cleansing in the occupied zone. Proper diffuser sizing, exhaust positioning, and commissioning visualization tests reduce this risk.
5) Exhaust System Engineering Requirements
In a negative pressure operating room, the exhaust system is not a secondary feature — it is the containment mechanism. When exhaust performance is unstable, negative pressure containment collapses immediately.
5.1 Dedicated exhaust system
A negative pressure OT should be equipped with a dedicated exhaust path (duct + fan + discharge), avoiding shared return systems or adjacent-room exhaust networks that could reintroduce contamination risk.
5.2 Exhaust airflow must exceed supply airflow
Negative pressure is achieved through controlled imbalance: Exhaust = Supply + (10–15%). In practice, exhaust should be controlled dynamically to maintain differential pressure stability during door events and filter loading.
5.3 HEPA filtration before discharge
In infectious or high-risk applications, exhaust air is typically filtered (HEPA) before being discharged outdoors to reduce environmental risk and protect maintenance personnel. Some high-containment designs use redundant filtration stages.
5.4 Backflow prevention
Backdraft dampers/check valves at discharge prevent reverse airflow during fan shutdown or wind-induced pressure reversal. This supports containment stability under transient conditions.
5.5 Discharge location and re-entrainment avoidance
Exhaust discharge should be positioned to avoid re-entrainment into building fresh air intakes. Rooftop discharge, adequate clearance, and careful intake separation are common requirements.
5.6 Failure strategy and reliability
Because containment depends on exhaust continuity, design often includes:
- Pressure alarms and fan fault alarms
- Optional redundancy for critical rooms
- Filter differential pressure monitoring
- BMS integration for tracking and compliance documentation
6) The “No Return vs Return” Debate
One of the most debated decisions in negative pressure OT design is whether to eliminate return air completely or allow controlled recirculation. Both approaches can be valid — the correct choice depends on infection risk profile, climate/energy constraints, and operational policy.
6.1 Philosophy A: No return air (100% fresh air + 100% exhaust)
In this approach, return air is eliminated. Air moves in a one-way path: Outdoor → AHU → Room → Exhaust → Outdoor. This offers the clearest containment logic because contaminated air is not recirculated.
Why it’s chosen: Maximum isolation margin, simplified infection-control defensibility, minimized risk of system cross-contamination.
Trade-offs: higher energy demand, increased dehumidification load (especially in humid climates), and larger AHU capacity requirements to maintain stable temperature and RH.
6.2 Philosophy B: Return + exhaust (controlled recirculation)
In this approach, return air is used (often for stability and energy reasons) while a dedicated exhaust system still creates negative pressure: Exhaust > Supply remains the governing rule.
Core condition: Return air must be isolated (typically via a dedicated AHU) and filtered appropriately; exhaust remains the containment driver.
Benefits: improved humidity and temperature stability, smaller required AHU capacity versus full 100% outdoor air systems, and reduced operational cost.
6.3 The core engineering truth
- Negative pressure is defined by exhaust dominance, not by the mere presence/absence of return grilles.
- Eliminating return does not guarantee containment if exhaust design is weak or controls are missing.
- Allowing return does not automatically reduce safety if return is isolated, filtered, and exhaust remains dominant.
6.4 When each strategy is typically used
| Decision Factor | No Return (100% OA + 100% Exhaust) | Return + Exhaust (Dedicated AHU) |
|---|---|---|
| Infection risk profile | High-containment infectious surgery priority | Occasional-use infectious capability / balanced approach |
| Energy & humidity constraints | Higher load, more complex RH stability | Better RH stability, lower OPEX |
| Defensibility / simplicity | Strongest “one-way air path” narrative | Requires clear isolation + filtration explanation |
| Typical project behavior | Used when policy prioritizes containment above all | Common when dedicated AHU is available and stability is critical |
7) Pressure Monitoring & Control Systems
Negative pressure is not achieved by design intent alone. It must be continuously measured, controlled, and verified. A pressure-controlled operating room is an active system — not a passive airflow imbalance.
7.1 Differential pressure monitoring
- Low-range differential pressure sensor (room vs corridor/anteroom)
- Continuous local display (at entrance) + alarm
- Trend logging (preferred) for compliance and troubleshooting
7.2 Active control logic
Typical control loop: Pressure sensor → controller → exhaust fan VFD or modulating dampers → pressure correction. Exhaust-driven control is often more stable because exhaust directly governs room pressure.
7.3 Door opening events and pressure recovery
Door events can temporarily collapse differential pressure. A well-tuned system should restore setpoint rapidly without oscillation. Practical commissioning should include door-event testing to verify recovery performance.
7.4 Alarm and interlock integration
Typical integrations include: BMS interface, exhaust fan fault alarm, pressure deviation alarm, and optional door access logic. The goal is immediate visibility when containment is not achieved.
7.5 Failure modes
- Exhaust fan failure or power loss
- HEPA filter blockage increasing static pressure
- Damper faults or sensor drift
- Envelope leakage changes over time
Engineering insight: A “negative pressure OT” without monitoring is not verifiable containment. It is a ventilation assumption.
8) Positive vs Negative Pressure Operating Rooms — Engineering Comparison
Positive and negative pressure strategies are designed to solve different risk scenarios. Understanding the differences prevents misapplication and supports correct tender specifications.
| Parameter | Positive Pressure Operating Room | Negative Pressure Operating Room |
|---|---|---|
| Primary objective | Protect sterile field / patient | Contain airborne contamination |
| Pressure relationship | Room higher than adjacent spaces | Room lower than adjacent spaces |
| Airflow direction | Outward (OR → corridor) | Inward (corridor → OR) |
| Airflow balance logic | Supply > Exhaust | Exhaust > Supply |
| Exhaust system role | Support ventilation balance | Primary containment mechanism |
| Return air | Common (recirculation) | Optional; debated; must be isolated if used |
| Monitoring requirement | Recommended | Critical (continuous DP + alarm) |
| Operational impact | Moderate energy demand | Often higher (especially 100% outdoor air designs) |
Simple memory rule: Positive pressure protects the patient. Negative pressure protects the environment.
9) Engineering Challenges in Modular Negative Pressure OT Implementation
Negative pressure rooms can look correct on paper but fail in real projects due to envelope leakage, poor balancing, or weak commissioning. In modular operating theatres, implementation requires cross-discipline coordination.
9.1 Envelope airtightness (modular joints and penetrations)
Pressure stability depends on envelope integrity. Typical leakage points include panel joints, ceiling interfaces, access panels, and MEP penetrations. A modular envelope must be treated as a pressure boundary, not just an architectural finish.
9.2 Door leakage and pressure recovery
Doors are dynamic leakage points. Poor sealing or misalignment can cause frequent pressure alarms and force higher exhaust compensation. Door quality, sealing design, and installation accuracy directly affect containment stability.
9.3 Duct routing constraints
Modular OTs often carry dense ceiling coordination (laminar ceiling, medical gas, electrical trays, surgical lights). Adding dedicated exhaust ducting can create spatial conflicts and airflow short-circuit risks if not coordinated early.
9.4 Balancing stability over time
Over time, filter loading increases pressure drop, dampers drift, and leakage can change. A robust system includes measurement points, control margin, and trend monitoring for stable performance.
9.5 Humidity control in tropical climates
In high-humidity regions, 100% outdoor air strategies can significantly increase dehumidification demand. AHU coil sizing, control tuning, and condensation risk management become critical to maintaining stable RH and comfort.
9.6 Commissioning and validation complexity
Negative pressure OTs should be validated by airflow measurement, pressure stability testing (including door-event tests), alarm validation, and smoke visualization to confirm inward airflow direction and avoid short-circuit patterns.
Common failure pattern: A room may pass a “static” balancing check but fail during real workflow (door opening, staff movement, filter loading).
10) Integrating Negative Pressure Strategy into Modular OT Systems
Negative pressure performance is achieved when architectural envelope, airflow organization, exhaust strategy, and control logic are designed as one integrated system. Modular operating theatres can support this well when integration is considered early.
10.1 Envelope integrity as a pressure-control component
- Sealed panel joints and defined sealing methods
- Gasketed access panels (not open inspection holes)
- Controlled penetrations for medical gas/electrical services
- Door-frame sealing integrated to wall system
10.2 Door systems for containment environments
Door sealing, closing behavior, and alignment directly affect pressure stability. In negative pressure applications, doors should be treated as containment interfaces, not only as architectural elements.
10.3 Coordinating laminar ceiling with exhaust placement
Exhaust placement must support contaminant capture while avoiding disruption to clean-zone supply patterns. In higher-risk rooms, dual-level exhaust strategies can improve capture behavior.
10.4 Dedicated AHU and smart monitoring integration
Dedicated AHU configuration enables independent balancing and supports more stable humidity control. Pressure displays, alarms, and BMS connectivity support predictable commissioning and long-term compliance.
ICARELIFE positioning (subtle): At ICARELIFE, negative pressure containment is engineered as part of a modular OT ecosystem — integrating envelope sealing, airflow strategy, exhaust containment, and pressure monitoring to support predictable handovers for contractors and engineering partners.
Planning a Containment-Ready Operating Theatre Project?
If you are a healthcare contractor, MEP partner, or cleanroom integrator, ICARELIFE can support your project with modular OT coordination: airtight envelope planning, exhaust/pressure logic, grille strategy, and commissioning-ready design inputs.
Note: Internal links above are placeholders — update them to your final ICARELIFE page URLs (e.g., AHU blog, laminar ceiling blog, hermetic door blog).
11) Frequently Asked Questions (FAQ)
What is the standard pressure differential for a negative pressure operating room?
Most negative pressure operating rooms are maintained at –5 Pa to –15 Pa relative to adjacent corridors or anterooms, with continuous monitoring and alarm integration.
How is negative pressure created in an operating room?
Negative pressure is created when exhaust airflow exceeds supply airflow (commonly by 10–15%), ensuring inward airflow from adjacent spaces.
Is return air allowed in a negative pressure operating room?
Return air may be allowed when served by a dedicated AHU and properly isolated/filtered. High-containment designs may eliminate return air entirely and operate on a 100% fresh air and 100% exhaust basis.
Is HEPA filtration required for exhaust air?
In infectious or high-risk applications, exhaust air is typically HEPA filtered before outdoor discharge to reduce environmental risk and protect maintenance personnel.
What happens if negative pressure fails?
If differential pressure drops below threshold, containment integrity is compromised. Pressure alarms, fan fault alarms, and rapid recovery control logic are critical.
Can a positive pressure operating room be converted to negative pressure?
Conversion is possible but requires rebalancing supply and exhaust airflow, installing a dedicated exhaust path, adding pressure monitoring, and verifying envelope airtightness.
How many air changes per hour (ACH) are required?
Negative pressure operating rooms typically operate around 15–25 ACH depending on standards. ACH supports dilution; negative pressure is achieved by exhaust dominance.
Does eliminating return air automatically improve safety?
Not automatically. Containment depends on exhaust design, filtration, control stability, and envelope integrity. Eliminating return increases containment margin but increases energy and humidity-control burden.
Why is a dedicated AHU recommended for negative pressure OTs?
A dedicated AHU helps isolate airflow control, improves humidity stability, reduces cross-room contamination risk, and simplifies balancing and verification.
Engineering Summary
Negative pressure operating rooms are containment-focused surgical environments. Real performance depends on exhaust system dominance, pressure monitoring and recovery behavior, envelope airtightness, and commissioning validation — not on airflow imbalance alone.
This article reflects practical HVAC integration experience across modular operating theatre projects and contractor workflows.