IVF Clinic Departments: Functions & Purpose of Every Room Explained
Every room inside an IVF clinic serves a precise, non-replaceable medical function. This guide covers all key IVF clinic departments — from embryology lab to cryostorage room, operating theater, and recovery area — with the design and environmental standards each one requires.
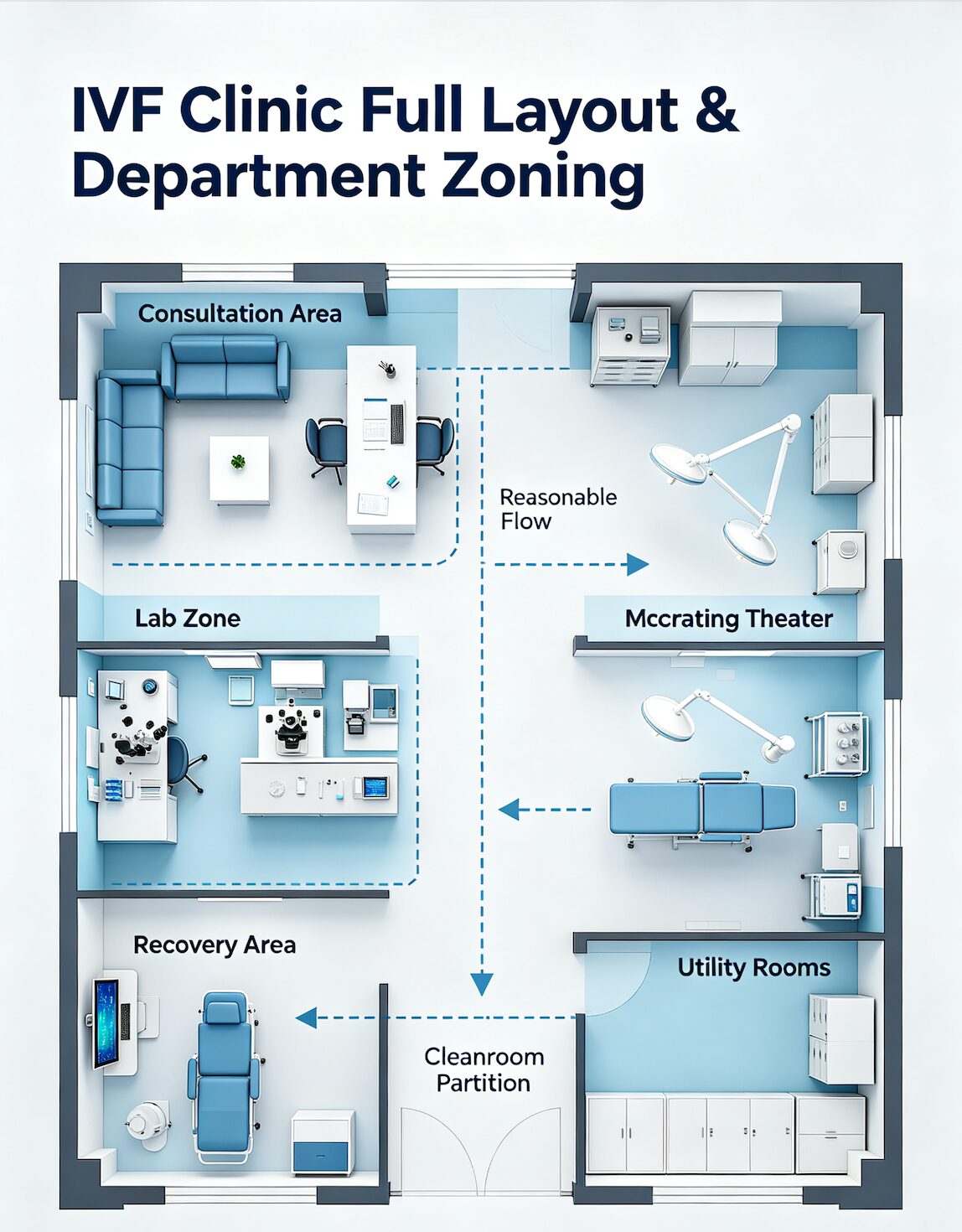
- IVF clinic departments include reception, semen collection room, andrology lab, embryology lab, cryostorage room, operating theater, sterilization room, recovery area, and utility support rooms.
- The embryology laboratory is the most controlled zone — positive-pressure cleanroom with HEPA filtration and ISO-classified air quality.
- Each room serves a unique, non-substitutable function; layout zoning directly affects IVF success rates and regulatory compliance.
- Environmental controls — temperature, humidity, air pressure, and particle count — must be maintained independently in each department.
- Facility designers, contractors, and clinic operators must plan each zone according to its specific contamination risk and workflow sequence.
An IVF clinic is one of the most strictly regulated medical facilities in the healthcare sector. Unlike general hospital wards, every IVF clinic department is purpose-built around controlled air quality, temperature stability, sterile zoning, and precise workflow segregation.
Each room serves a unique, non-replaceable function in the fertility treatment process — from patient consultation and specimen collection, to embryo culture, cryopreservation, and surgical procedures. Understanding the layout and purpose of each IVF clinic department helps patients recognize clinic quality, and gives facility designers and medical teams the context to maintain compliant, high-success-rate operations.
Laboratory Zones
Embryology lab, andrology lab, and cryostorage — highest environmental control requirements in the clinic.
Clinical Zones
Operating theater, scrub room, and recovery area — surgical-grade sterility and post-procedure monitoring.
Support Zones
Sterilization room, semen collection room, and sterile storage — infection control and supply continuity.
Utility & Admin Zones
Medical gas rooms, UPS rooms, staff changing, and document management — operational backbone of the clinic.
1. Reception & Consultation Area
The public-facing front-end of the IVF clinic — designed for patient admission, private consultation, and treatment planning before any clinical procedure begins.

Core Functions
- Receive and register new and returning fertility patients
- Conduct private one-on-one fertility consultations with clinicians
- Explain IVF treatment cycles, procedures, risks, and success rate expectations
- Store and manage patient medical records and signed consent documentation
2. Semen Collection Room
A private, enclosed, medically controlled room dedicated exclusively to male specimen collection — positioned immediately adjacent to the andrology laboratory for direct sample handover.
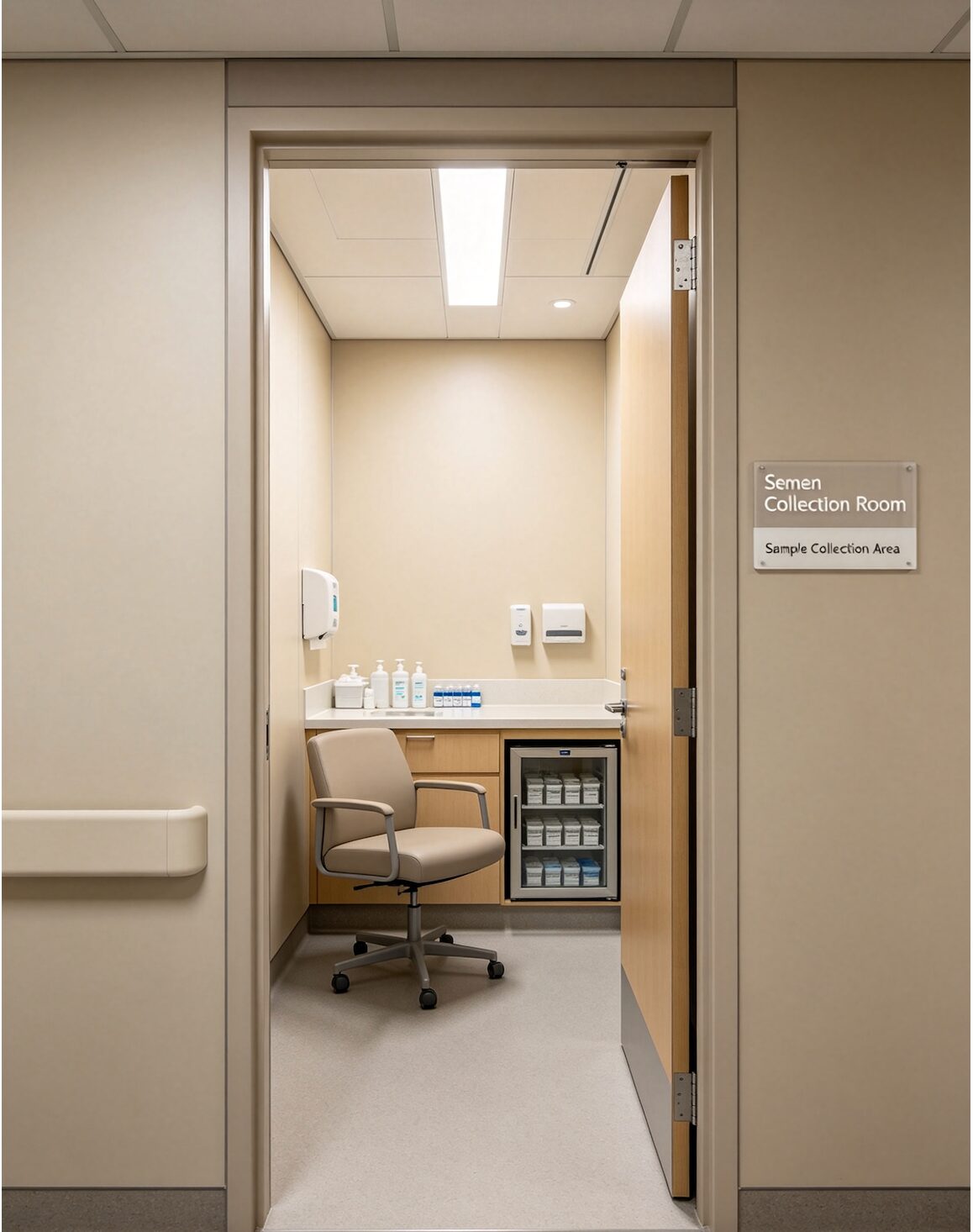
Core Functions
- Provide a quiet, hygienic, and fully confidential environment for sample collection
- Ensure collected specimens remain uncontaminated before laboratory processing
- Enable immediate transfer of fresh samples to the andrology lab — time-sensitive after collection
3. Andrology Laboratory
The primary male fertility testing and sperm processing laboratory. All sperm-related diagnostic, preparation, and cryopreservation work is handled exclusively here.

Core Functions
- Perform full semen analysis — sperm count, motility, morphology, and vitality assessment
- Purify and prepare sperm samples for IVF and ICSI fertilization procedures
- Process sperm cryopreservation and prepare samples for long-term storage
- Maintain stable temperature, humidity, and clean air conditions to preserve sperm viability throughout processing
4. Embryology Laboratory
The core cleanroom heart of the entire IVF facility — and the most strictly controlled zone due to the extreme fragility of human embryos at every developmental stage.

Core Functions
- Perform in vitro fertilization (IVF) and intracytoplasmic sperm injection (ICSI)
- Culture, monitor, and grade embryo development from Day 1 through blastocyst stage
- Select high-quality embryos for embryo transfer based on morphological grading
- Prepare embryos for vitrification (freezing) or direct fresh-cycle transfer
Environmental Standards
| Parameter | Requirement | Reason |
|---|---|---|
| Air Classification | ISO Class 5–7 (cleanroom) | Eliminate airborne particle contamination near embryo workstations |
| Air Pressure | Positive pressure vs. adjacent zones | Prevent inward airflow and cross-contamination |
| Filtration | HEPA (H13/H14) via FFU units | Remove 99.97%+ of particles ≥0.3 µm |
| Temperature | 23–25°C stable | Match embryo incubator conditions; avoid thermal shock |
| Humidity | 40–60% RH | Prevent media evaporation and static charge buildup |
| VOC Control | Activated carbon filtration | Eliminate solvents, adhesives, and cleaning agent residues |
- Positive pressure failure allows airborne bacteria to enter embryo workstation zones
- VOC contamination from wall finishes or cleaning agents directly impairs embryo development
- Temperature instability stresses embryos during culture — even ±1°C deviation is significant
- Inadequate HEPA filtration leads to failed ISO classification during accreditation audits
Modular Cleanroom & Laboratory Systems by ICARELIFE
ICARELIFE supplies complete modular cleanroom systems including FFU ceiling arrays, positive-pressure AHU configurations, hygienic wall panels, and hermetic doors — pre-engineered for IVF laboratory compliance.
5. Cryostorage Room
A specialized low-temperature preservation room designed for long-term storage of frozen embryos, oocytes, and sperm in liquid nitrogen tanks — isolated from all general laboratory areas.

Core Functions
- Store frozen embryos, sperm, and oocytes in liquid nitrogen tanks at approximately −196°C
- Maintain consistent ultra-low temperature for long-term specimen viability across multiple treatment cycles
- Manage specimen labeling, patient traceability, and secure inventory records
- Isolate cryogenic equipment from general lab areas to prevent nitrogen vapor exposure and safety hazards
6. Operating Theater & Surgical Scrub Area
A high-grade sterile surgical room for all invasive fertility procedures — oocyte retrieval and embryo transfer — with an attached scrub room functioning as a sterile buffer zone for medical staff.
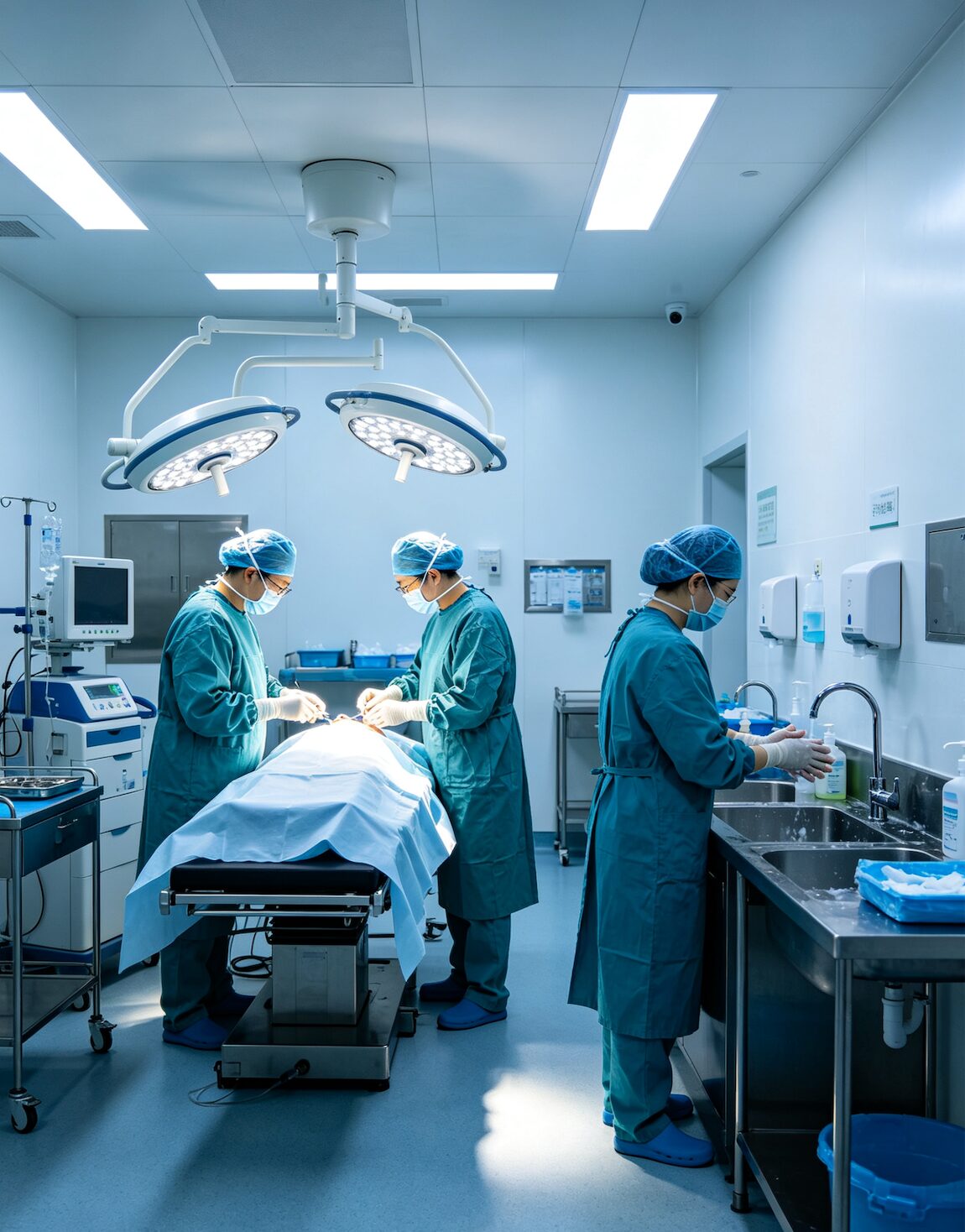
Operating Theater — Core Functions
- Perform ultrasound-guided oocyte retrieval (egg pickup procedures)
- Conduct fresh and frozen embryo transfer procedures under clinical supervision
- Maintain surgical-grade sterile air filtration, stable temperature, and positive-pressure airflow
Scrub Room — Core Functions
- Provide a dedicated space for surgical hand washing, gowning, and sterile preparation before OR entry
- Act as a contamination buffer between corridor areas and the sterile OR environment
- Laminar airflow ceiling — same standard
- Positive pressure differential — same standard
- HEPA H13/H14 filtration — same standard
- VOC-free finishes additionally required for IVF
- Proximity to embryology lab — IVF-specific requirement
- Direct connection or pass-through to embryology lab
- Hermetic sliding doors for pressure integrity
- Built-in medical gas supply (O₂, N₂O, medical air, vacuum)
- Instrument lighting compatible with ultrasound equipment
- Washable, non-porous wall and ceiling system
7. Cleaning, Sterilization & Sterile Storage Room
The infection control backbone of the IVF clinic — ensuring complete decontamination of reusable instruments and contamination-free storage of sterile equipment before use.

Core Functions
- Clean, disinfect, and autoclave reusable surgical and laboratory instruments
- Eliminate bacteria and biological residues from all medical tools using validated sterilization cycles
- Store fully sterilized equipment in dry, sealed, contamination-free conditions until point of use
- Maintain complete separation between contaminated (soiled) and clean (sterile) workflows
8. Patient Recovery Area
A quiet, monitored resting zone for patients after oocyte retrieval and embryo transfer procedures — providing clinical observation before patient discharge.

Core Functions
- Monitor patient vital signs and physical condition following surgical procedures
- Provide comfortable, supervised resting space before patient discharge
- Allow nursing staff to observe and respond to post-procedural side effects — including pain, bleeding, or nausea
9. Utility, Technical & Administrative Rooms
A fully functional IVF clinic depends on behind-the-scenes support infrastructure to sustain continuous, safe clinical and laboratory operations around the clock.

Key Supporting Rooms and Functions
- 1Staff Changing Rooms — Clean zone access control for all clinical and laboratory staff. Prevents external contamination from entering restricted areas via clothing or footwear.
- 2Medical Gas Room — Houses centralized medical gas supply systems (O₂, N₂O, CO₂, medical air, vacuum) for surgical and laboratory equipment. Requires fire-rated enclosure and pressure monitoring.
- 3UPS / Power Backup Room — Uninterruptible power supply protecting all sensitive embryology lab incubators, cryostorage alarms, and clinical monitoring systems from power disruption.
- 4AHU Plant Room — Houses the air handling unit supplying filtered, temperature-controlled, and humidity-controlled air to all laboratory and clinical zones. Requires 24/7 operational monitoring.
- 5Administrative & Document Room — Manages patient medical records, regulatory compliance files, treatment cycle documentation, and clinic accreditation records in secure, organized storage.
- 01 Modular Operating Theatre System OR Design
- 02 Laminar Airflow Ceiling Unit Cleanroom
- 03 Compact Modular AHU HVAC
- 04 Hermetic Sliding Doors Pressure Control
- 05 Corian Hygienic Wall Panels Wall System
Frequently Asked Questions
The embryology laboratory is generally considered the most critical department in an IVF clinic. It is where fertilization, embryo culture, and embryo grading take place — all in a strictly controlled cleanroom environment. Air quality, temperature stability, and VOC-free conditions in the embryology lab directly determine IVF success rates.
An embryology lab is a positive-pressure cleanroom where IVF and ICSI fertilization procedures are performed, embryos are cultured in CO₂ incubators, and embryo development is monitored and graded daily. It requires HEPA filtration, ISO-classified air quality, VOC-free wall finishes, and stable temperature and humidity control. It is typically the most restricted zone in the entire IVF facility.
The andrology lab is responsible for all male fertility testing and sperm processing. Functions include semen analysis (count, motility, morphology), sperm preparation for IVF and ICSI procedures, and sperm cryopreservation. It operates in a controlled environment adjacent to the semen collection room, and its outputs feed directly into the embryology lab for fertilization procedures.
The cryostorage room houses liquid nitrogen dewars for long-term frozen storage of embryos, oocytes, and sperm at approximately −196°C. It provides secure, labeled specimen management with traceability, and must be isolated from general lab areas due to nitrogen vapor hazards. Continuous oxygen monitoring and alarm systems are essential safety requirements for this room.
IVF embryology labs typically target ISO Class 5 at the embryo workstation level and ISO Class 6–7 for the surrounding lab space. Key requirements include HEPA H13/H14 filtration via FFU (Fan Filter Unit) arrays, positive pressure relative to adjacent zones, temperature control at 23–25°C, humidity at 40–60% RH, and activated carbon filtration to eliminate VOCs from the air supply.
An IVF operating theater meets the same laminar airflow, positive pressure, and HEPA filtration standards as a standard surgical OR. The key differences are its proximity to the embryology lab (to minimize embryo and oocyte transit time), the requirement for VOC-free wall and ceiling materials, and specific lighting and space requirements for ultrasound-guided egg retrieval procedures. Hermetic sliding doors are used to maintain pressure integrity between the OR and scrub areas.
A power failure in an IVF clinic without UPS backup can cause embryo incubators to lose temperature control — potentially destroying embryos in active culture cycles. It can also disable cryostorage monitoring alarms, leaving frozen specimens unprotected. Full UPS coverage for laboratory zones is a regulatory requirement in most healthcare accreditation frameworks and is considered a non-negotiable safety measure in any IVF facility design.
Summary: Every IVF Department Has a Precise Purpose
Every department inside an IVF clinic exists to serve a specific, non-interchangeable medical function. From patient consultation and specimen collection, through embryo culture and cryopreservation, to sterile surgery and post-procedure recovery — each room’s design, air quality control, and physical zoning directly influences patient safety and clinical outcomes.
For facility designers, contractors, and clinic operators, understanding these functional zones is the foundation of compliant, high-standard IVF laboratory and clinical facility planning. Room positioning, environmental specification, and workflow sequencing must all be coordinated from the earliest design phase.
Planning an IVF Clinic or Fertility Centre?
ICARELIFE supplies complete modular cleanroom systems, laminar airflow ceilings, hermetic doors, and AHU solutions pre-engineered for IVF laboratory and surgical zone compliance. Send your project brief and our technical team will respond with a system recommendation.